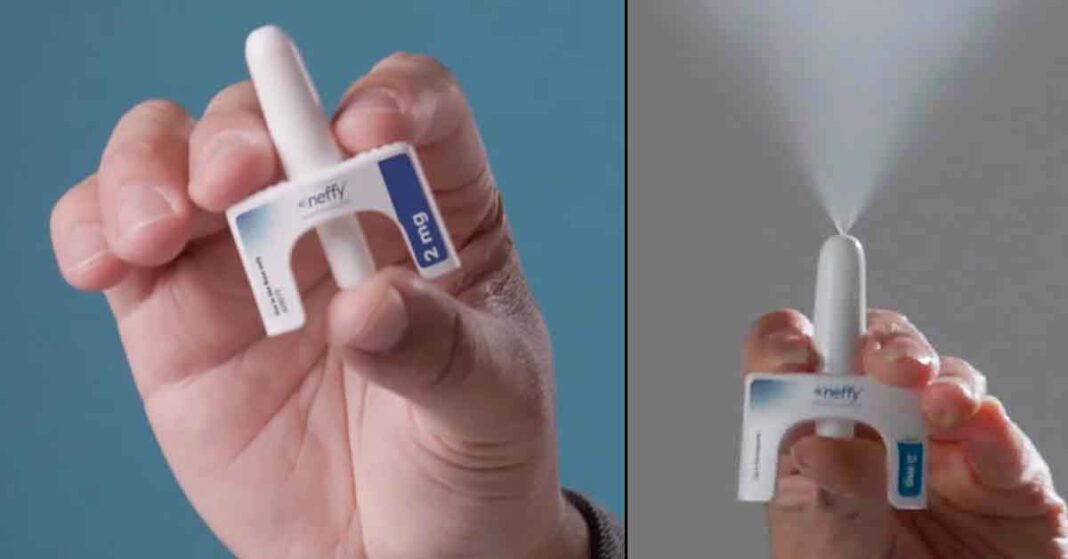
The recent shift in emergency allergy treatment has reached a significant milestone, as new data highlights a strong patient and caregiver preference for intranasal epinephrine over traditional needle-based delivery. In an interview with HCPLive, Douglas Mack, MD, a pediatric allergist and clinical assistant professor at McMaster University, discussed the clinical implications of the recently FDA-approved Neffy (epinephrine nasal spray). The data suggests that the ease of use and reduced anxiety associated with a needle-free option could fundamentally change how anaphylaxis is managed in real-world settings.
For decades, the epinephrine auto-injector has been the gold standard for treating life-threatening allergic reactions, yet it has long been hindered by “needle phobia” and the physical bulk of the devices. Dr Mack emphasized that the nasal spray addresses these psychological barriers, stating, “What we find is that the needle is a huge barrier for patients. Not just the pain of the needle, but the fear of the needle, and the fear of doing it wrong.” This hesitation often leads to dangerous delays in administering the life-saving medication during an emergency.
Research comparing the two delivery methods showed a dramatic preference for the nasal route. According to Mack, when patients and caregivers were given the choice and understood the efficacy was comparable, the vast majority opted for the spray. He noted, “When you look at the preference data, it’s overwhelmingly in favor of the nasal spray. It’s about 80% to 90% of patients who would prefer a nasal spray over an injection.” This preference is not merely a matter of comfort; it is a clinical advantage that ensures the medication is actually used when needed.
A critical component of this transition is the device’s portability and the simplicity of its administration. Unlike auto-injectors, which require specific positioning and force, the nasal spray is intuitive. Dr Mack pointed out that the compact nature of the device makes it more likely for adolescents and active adults to carry it consistently. “The portability is a game changer,” Mack explained. “If you have a device that fits in your pocket rather than something you have to carry in a bag, you’re much more likely to have it with you at the moment of truth.”
The clinical efficacy of the nasal spray has been a point of rigorous study, as it must achieve the same rapid absorption as an intramuscular injection to be effective during anaphylaxis. Dr Mack highlighted that the pharmacokinetics of the nasal spray are robust, providing reassurance to healthcare providers who might be skeptical of moving away from needles. He stated, “The data shows that we’re getting epinephrine levels that are comparable to what we see with the 0.3 mg auto-injector, which is the standard of care.”
Despite the enthusiasm, Dr Mack cautioned that education remains vital during this transition. Patients must understand that while the delivery method has changed, the urgency of the condition remains the same. The introduction of Neffy allows for a broader conversation about allergy safety, moving the focus from the “fear of the poke” to the “readiness of the response.” Mack observed that the spray helps “normalize” the treatment, making it feel less like a medical procedure and more like a standard safety precaution.
Ultimately, the move toward intranasal epinephrine represents a patient-centered evolution in immunology. By removing the primary barrier to administration—the needle—specialists like Dr Mack believe that outcomes for anaphylaxis will improve through faster intervention. As Mack concluded, “At the end of the day, the best epinephrine is the one that actually gets given. If this device removes the barrier to giving it, then we’ve made a massive step forward in patient safety.”
ARS Pharma, which markets neffy, is an advertiser with SnackSafely