HOUSTON, Nov. 10, 2019 /PRNewswire/ — Bryn Pharma, LLC (“Bryn” or the “Company”), a privately held pharmaceutical company dedicated to finding a better way for patients and caregivers to treat anaphylaxis, announced that the results of two studies supporting the potential benefits of its BRYN-NDS1C product candidate, Bi-dose Epinephrine Nasal Spray, were presented today at the Annual Scientific Meeting of the American College of Asthma, Allergy and Immunology (ACAAI) in Houston, TX.
Results from a study evaluating the impact of nasal congestion on epinephrine pharmacokinetics (PK) and heart rate after intranasal epinephrine administration demonstrated that histamine-induced nasal congestion, a common symptom seen in patients experiencing an anaphylactic event, increased the absorption of intranasal epinephrine and led to a more rapidly increased heart rate.
“Since histamine is released during the immunologic cascade of events associated with an anaphylactic reaction which leads to nasal congestion, a key focus of our pre-clinical program was to demonstrate that administering epinephrine intranasally to a congested patient doesn’t interfere with the delivery of the drug,” said David Dworaczyk, Ph.D., CEO of Bryn Pharma. “The results presented today demonstrated that epinephrine was absorbed more rapidly in this pre-clinical congestion model. We are looking forward to completing our clinical program shortly.”
In a second presentation at the ACAAI meeting today, researchers presented results from a multicenter, randomized preference study which demonstrated that healthcare professionals had a statistically significant preference for BRYN-NDS1C over the EpiPen® Auto-Injector for all study metrics, including ease of use, portability and safety. The researchers also concluded, considering that the most common cause of death from food allergies is delayed epinephrine administration, prescription and use of BRYN-NDS1C might decrease the incidence of anaphylactic deaths. These findings are consistent with the results of a study presented at the American Academy of Pediatrics Conference last month demonstrating patient preference for the product candidate, BRYN-NDS1C, versus EpiPen® Auto-Injector. HCP preference for BRYN-NDS1C was evaluated across a series of key parameters including:
| Question | Preference for ENS Device, n (%)(N=56) | p-value |
| Which device do you think a patient would be more likely to carry with them in daily life? | 50(89.3) | <.001 |
| Which device do you think would be easier for patients to learn how to use? | 43(76.8) | <.001 |
| Which device is easier to use? | 46(82.1) | <.001 |
| Which device do you prefer overall? | 38(67.9) | <.001 |
| Which device would you recommend to patients? | 37(66.1) | <.001 |
| Which device do you think would be safer for a patient to use? | 39(69.6) | <.001 |
| Which device do you prefer based on the size of the device? | 46(82.1) | <.001 |
| Which device do you think a patient would be more likely to use in a real emergency? | 29(51.8) | .003 |
Dworaczyk added, “We are also pleased to share results from our follow-on, healthcare professional preference study with those at the forefront of allergy care. This study, which aligns with our patient preference data, suggests that the use of Bryn’s Bi-dose Epinephrine Nasal Spray instead of the Epinephrine Auto-Injector for the treatment of anaphylaxis may increase patient adherence, decrease the time to treat symptoms and potentially reduce hospitalization and anaphylactic deaths.”
About the Studies
Nasal Congestion Study
Three dogs participated in a nasal congestion pilot study to assess the effects of INH on nasal congestion response in dogs compared with intranasal saline administration. Anesthetized dogs received a single dose of 5 percent histamine. Intranasal histamine increased nasal pressure at 60, 80 and 100 minutes after dose.
After the pilot study, the effects of intranasal epinephrine on epinephrine pharmacokinetics and heart rate were evaluated in two groups (histamine versus saline) consisting of six dogs each. Anesthetized dogs received either a single intranasal dose of 5 percent histamine or nebulized saline followed by a single intranasal epinephrine dose (4 mg/100 µL). Changes in nasal pressure were measured at varying intervals from 0 to 130 minutes. During this study, no animals were injured, and all dogs were adopted into foster homes once the study was completed.
Pharmacokinetics
- Blood sampling was performed before dosing and at set time points up to 130 minutes.
- Histamine administration produced a higher peak epinephrine concentration (Cmax) of 3.5ng/mL versus 1.7ng/mL in the saline group following IN epinephrine (p=0.06)
- Significantly lower Tmax occurred in the histamine versus saline group after receipt of intranasal epinephrine (six vs 70 minutes; p=0.02)
- After intranasal epinephrine, AUC1-90 was increased in dogs that received histamine versus saline (117 vs 59 ng/mL *minutes, respectively, p=0.09)
Heart Rate
- After intranasal epinephrine, the histamine versus saline groups showed immediate (5 minutes) versus delayed (30-60 minutes) increases in heart rate, respectively.
Healthcare Professional Preference Study
In a multi-center, randomized crossover preference study of Bi-dose Epinephrine Nasal Spray versus EAI, preference was evaluated in an eight-item, forced-choice questionnaire that was developed based on differences between the Bi-dose Epinephrine Nasal Spray and EAI for epinephrine administration. Two user groups participated in the preference study including 56 patients with severe allergies (results from the patient preference study were previously presented) and 56 healthcare professionals who treat patients with severe allergies (15 primary care physicians, 15 allergy/immunology physicians, 16 primary care nurses/trainers, and 10 allergy/immunology nurses/trainers). Participants attended a one-on-one session to learn how to use both devices. After using both training devices, participants completed an eight-item questionnaire.
The assessment of preference was based on the following metrics: ease of patient training, ease of use, portability, safety, comfort, size and emergency. For all metrics evaluated, the survey results indicated a statistically significant preference for the Bi-dose Epinephrine Nasal Spray over the EAI.
About the Clinical Development Program for BRYN-NDS1C
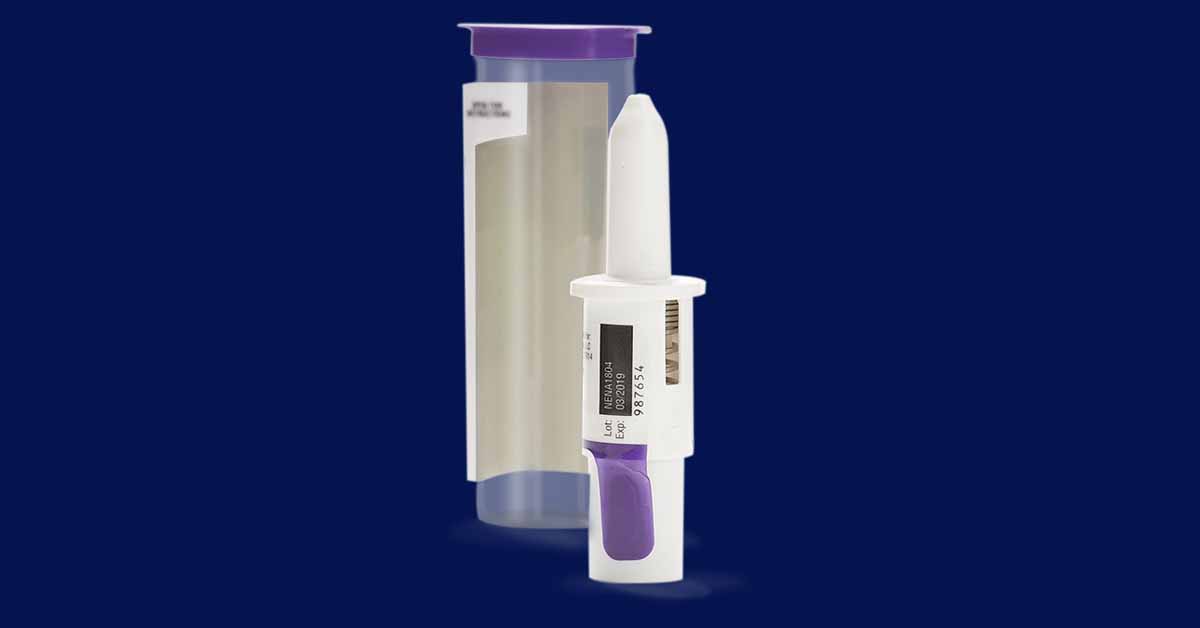
Bryn’s Bi-dose Epinephrine Nasal Spray (BRYN-NDS1C) is a single, portable, needle-free device capable of delivering two therapeutic doses of epinephrine, replacing the need to carry two epinephrine auto-injectors. In early 2019, the U.S. Food and Drug Administration (FDA) granted Fast Track Designation to BRYN-NDS1C. In October 2019 the Company completed dosing in the pivotal human trial designed to support U.S. approval to market the product candidate. BRYN-NDS1C is not currently approved for sale by the FDA or any international regulatory authority.
About Anaphylaxis
Anaphylaxis is a serious, life-threatening allergic reaction. The most common anaphylactic reactions are to foods, insect stings, medication and latex.1 A major difference between anaphylaxis and other allergic reactions is that anaphylaxis typically involves more than one system of the body.2 Anaphylaxis requires immediate medical treatment, driving approximately 100,000 emergency room visits in the U.S. each year.1,3 Because 30 percent of patients who develop anaphylaxis will require a second dose of epinephrine to control symptoms, practice parameters recommend that physicians provide patients with two auto-injectors.4 If not treated properly, anaphylaxis can be fatal.2 However, studies have shown that the majority of people at risk for anaphylaxis often do not carry two Epinephrine Auto-Injectors due in part to size and cost of the products, putting patients at greater risk of severe complications during an allergic reaction.
About Bryn Pharma
Bryn Pharma, founded in 2016, is a privately held pharmaceutical company founded by patients for patients. Bryn is focused on positively disrupting the existing market for epinephrine auto-injectors by delivering an accessible, easy-to-use alternative that better meets the needs of patients. Bryn Pharma seeks to provide this growing population at risk for anaphylaxis with A Better Way to be prepared for a life-threatening allergic reaction. For more information visit www.brynpharma.com.
EpiPen is a registered trademark of Mylan Inc.
Forward-Looking Statements
Statements made in this press release that look forward in time or that express beliefs, expectations or hopes regarding future occurrences or anticipated outcomes or benefits are forward-looking statements. A number of risks and uncertainties, such as risks related to product development and commercialization efforts, results of clinical trials, ultimate clinical outcomes and benefit of the Company’s products to patients, market and physician acceptance of the Company’s products, intellectual property protection and competitive product offerings, could cause actual events to differ from the expectations indicated in these forward-looking statements. You are cautioned not to put any undue reliance on any forward-looking statement. This press release is neither an offer to sell nor a solicitation of an offer to purchase any particular securities. Any such offer or solicitation will be made only pursuant to definitive legal agreements prepared specifically for such purpose. An investment in the Company’s securities entails significant risks and is suitable only for sophisticated investors who can afford a loss of their entire investment; no assurance can be given that investment objectives will be achieved. In considering the performance information contained herein, you should bear in mind that past performance is not necessarily indicative of future results; there can be no assurance that the Company will achieve comparable results or that any projected returns will be met. The Company does not assume any obligation to publicly update or revise any forward-looking statements, whether as a result of new information, future events, or otherwise.
- American Academy of Allergy, Asthma & Immunology. Available at https://www.aaaai.org/conditions-and-treatments/allergies/anaphylaxis. Accessed on June 19, 2019.
- American Academy of Allergy, Asthma & Immunology. Available at: https://www.aaaai.org/conditions-and-treatments/conditions-dictionary/anaphylaxis. Accessed on June 19, 2019.
- Fromer L. Prevention of Anaphylaxis: The Role of the Epinephrine Auto-Injector. Am J Med. 2016 Dec; 129(12): 1244-1250.
- Anaphylaxis – a practice parameter update 2015; Lieberman, Phillip et al.; Annals of Allergy, Asthma & Immunology, Volume 115, Issue 5, 341-384.
Spokin’s Omission of Crucial Allergen Processing Information Puts Allergic Individuals at Risk